Using CBD Oil for chronic pain is becoming more popular around the world. This trend is increasing in Australia since laws were introduced to allow doctors to prescribe medicinal cannabis.
Chronic pain is an uncomfortable and undesirable medical illness that causes a lot of suffering to roughly 3.4 million Australians. Furthermore, 1 in 5 people aged over 45 continue to live with chronic pain. In 2015, it was estimated that around 20 percent of the population lives with chronic pain, proving it to be incredibly common.
In Australia, the number of people living with chronic pain visiting general practitioners has risen by 67 percent over the past 10 years.
Whilst many people experience pain due to various reasons, it is only characterised as being chronic if it persists or recurs for an extended period of time for longer than three months. Chronic pain can be subjective, in that every person has a different experience of pain. This can make it difficult for doctors to diagnose, however patients suffering from chronic pain generally experience moderate to high levels of pain daily for months or years at a time.
Chronic pain is a common experience in the healing time after an illness or injury which is normally around 3 to 6 months. Some of the more common chronic illnesses include: migraines, arthritis, osteoporosis and endometriosis.
It is essential to distinguish between chronic and acute pain. Acute pain tends to be more sudden, short-term (a few days or weeks), and has a sharp pain sensation, which usually disappears after the injury heals. It can occur due to an injury or illness where body tissue may be damaged or swelling occurs. Acute pain often serves as a useful warning that something is causing damage to the body.
Chronic pain is caused by many different things. Chronic pain may be the result of an injury, or brought on due to the presence of other medical illness. The most common causes include:
Some types of chronic pain include:
Risk factors that contribute to the overall likelihood of developing chronic pain include:
Research from the British Journal of Pain has found connections between lifestyle and the chances of acquiring chronic pain. The study found that people can prevent and manage chronic pain by modifying the following lifestyle and behavioural factors:
Limit your opportunities to be injured. Acute pain is one of the most critical risk factors for chronic pain. Depending on how painful it is and the number of locations it is experienced in, the likelihood of developing chronic pain increases. Additionally, if you suffer from other chronic conditions, you are more likely to suffer from long-term chronic pain.
If you are overweight or obese face more risk of running into chronic pain later in life due to the greater pressure on their joints and muscles. This intensity from this pain can affect your ability to move or perform tasks, which consequently impacts your quality of life.
A lack of physical exercise is linked to chronic pain. Exercising regularly may help decrease pain and increase your mobility. As a result, your overall quality is likely to improve. It is recommended that chronic pain sufferers use tailored exercise programs to suit their individual needs for effective pain management.
Smokers are more likely to develop chronic illnesses such as Fibromyalgia. Heavy smokers experience more pain points with increased intensity than people who have never smoked.
Despite being popular for its temporary analgesic (pain relieving) effects, people who consume above the recommended daily amount of alcohol can experience greater pain sensitivity and intensity. This effect can also occur when people withdraw from drinking.
Disruptions to your sleep is noted as a factor that determines whether someone may develop chronic pain.

Pain intensity, distress and impact on bodily functions form an indication of pain severity. Some cases are so severe that they result in a physical or mental disability. In fact, chronic pain is one of the leading causes of disability around the world.
Chronic pain affects you in more ways than just the pain itself. People living with chronic pain often suffer physically, psychologically and socially. This could include your ability to:
Consequently, sufferers of chronic pain are also more likely to develop mental health issues, such as depression, anxiety and insomnia.
Chronic pain requires a lot of emotion and physical energy. As such, you may feel a range of symptoms that affect your quality of life including:
Chronic pain can be complex and experience of pain is somewhat subjective. As a result, medical professionals can find it difficult to eliminate completely. Consequently, doctors usually offer a range of treatments to reduce pain, increase function and improve the overall quality of life of their patients. A mix of therapies and medication is often used to treat chronic pain as the experience affects both mental and physical wellbeing.
Pharmacological treatments include a range of analgesics to manage and relieve chronic pain symptoms. Some of these analgesics include:
Non-pharmacological therapy can also help manage chronic pain and have proven effective in conjunction with pain medication. Some of the most common options are:
Complementary and alternative medicine is increasing in popularity amongst chronic pain patients. A survey of 908 people living with chronic pain revealed 27 to 60% use complementary and alternative medicine over conventional treatments. Medicinal cannabis and CBD is one such alternative medicine.
The reputation of Cannabidiol (CBD) for its various medicinal effects continues to grow. The cannabis plant, known as Cannabis sativa, contains over 500 chemicals, including phytocannabinoids. CBD is one of two major phytocannabinoids (alongside THC) which CBD can be extracted to produce medicinal CBD oil.
One of the benefits of CBD is that it does not make you high. Having said that, CBD does has several medicinal effects that are beneficial for pain management:
Ultimately, interest and application of medicinal CBD for chronic pain continues to increase, as a result of its neuropathic analgesic effects. A study in Frontiers in Pharmacology found that CBD is effective at reducing pain by over 30% in patients with Fibromyalgia.
A 2018 study of 1,483 medicinal CBD patients reported over 700 respondents were using CBD to treat chronic pain. 35.8% of participants also claimed that CBD treated their medical condition “very well by itself.” This includes the top three conditions listed below – chronic pain, arthritis/joint pain, and anxiety.
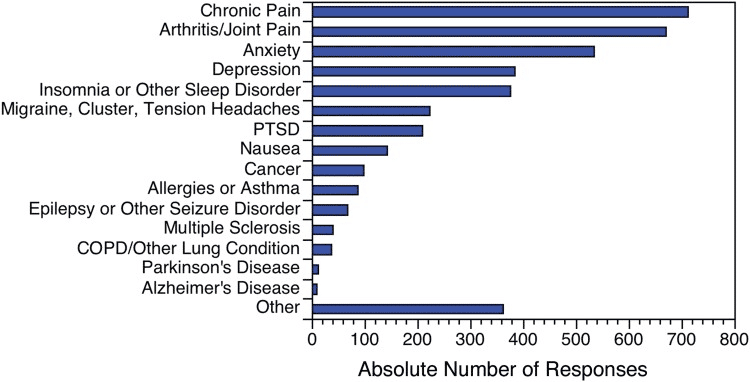
These findings suggests that CBD has the ability to help with chronic pain management. As always, you should speak to your doctor to determine whether CBD is appropriate for your individual needs.
Currently, doctors prescribe CBD and medical cannabis for various chronic pain related illnesses. These include:
Countries such as Canada and the United States already approve the use of cannabinoids as medicinal treatments. The main reason for its approval in Canada is due to the pain-relief offered by CBD, especially in treatment of chronic neuropathic pain.
A 2018 survey of 2,032 medicinal cannabis users found that 42.2% (861 people) used CBD to treat pain syndromes. Of these respondents, 598 were patients suffering with chronic pain.
CBD is increasing in acceptance across the world. Much of this acceptance can be attributed to breakthrough treatments helping epilepsy suffers due to its anti-convulsive properties.
Since its origins as a potential epilepsy remedy, CBD has gained international attention for other medicinal benefits. In 2017, the World Health Organisation (WHO) officially exonerated CBD as a substance of abuse or dependence. Furthermore the WHO advises that there are no other wider public health concerns around its use.
A few months later in 2018, the World Anti-Doping Agency (WADA) removed CBD from its prohibited list due to its anti-inflammatory and pain-relieving effects. It also asserted that CBD may be hundreds of times more powerful than the effects of aspirin.
Although there have been several studies that suggest CBD Oil for chronic pain can be effective, more long-term human research is required.
That said, medicinal CBD shows promising signs as an effective treatment for pain. The bulk of scientific and anecdotal reports available suggests that CBD may assist people in managing their chronic pain symptoms.
CBD oil is a safe alternative to THC, as it does not have intoxicating effects and a lower risk profile than many other pain medications.
As always, you should speak with your doctor before using CBD oil or any prescription medication.





















Stay up to date with medicinal CBD and alternative medicine in Australia.